Has chronic pain caused global concern? What is chronic pain? What are the causes of chronic pain? How is chronic pain managed? There is no better treatment for patients with chronic pain than empathy (putting oneself in another person’s position) and understanding from the physiotherapist and the patient’s family.
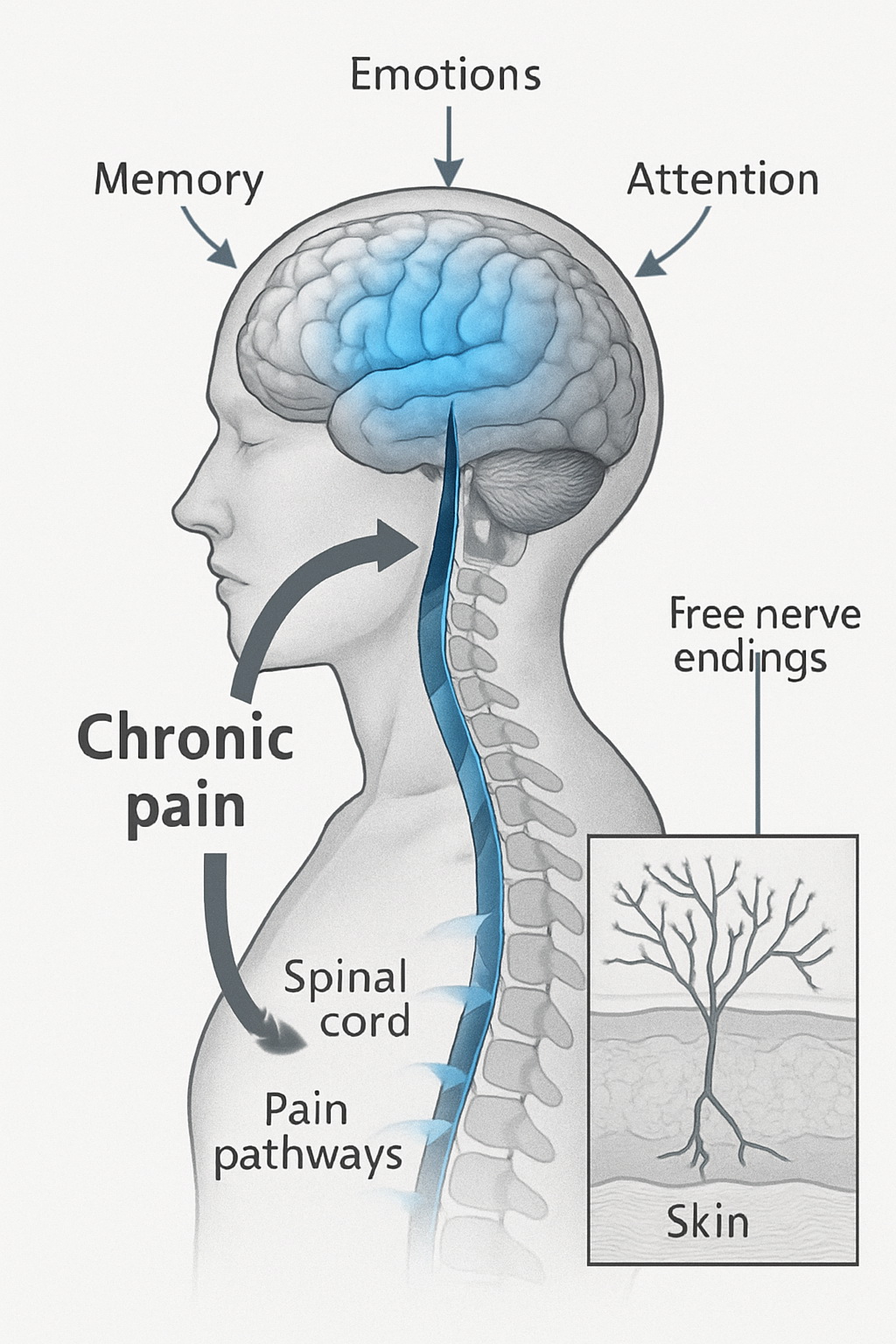
Pain is a sensory and emotional experience that varies among individuals, depending on the meaning attributed to pain and the person’s psychological state.
Has Chronic Pain Become a Global Concern?
Chronic pain is a major public health concern worldwide. Multiple pathways within the Central Nervous System (CNS)—namely the brain and spinal cord—are involved in pain processing.
Cognitive and emotional factors significantly influence pain perception, and these relationships are linked to interconnected brain regions that can modulate pain. In simple terms, a negative emotional state can intensify pain, while positive thinking may reduce it. Similarly, cognitive states such as attention and memory can either increase or decrease pain perception.
What Is Chronic Pain?
Chronic pain is defined as pain that persists beyond the normal tissue healing time following injury or inflammation and is generally considered to be pain lasting longer than 12 weeks.
What Are the Causes of Chronic Pain?
Chronic pain conditions may be recognized as having:
• An identifiable pathological, genetic, or biological origin
This includes conditions with hereditary or biological causes that explain symptom presentation, such as osteoarthritis, rheumatoid arthritis, systemic inflammatory rheumatic diseases, and connective tissue disorders. These conditions are typically diagnosed through objective biological or inflammatory markers, imaging findings, or identifiable tissue damage.
or
• An idiopathic origin (unknown pathological cause)
This is often based on subjective patient reporting and includes conditions such as complex regional pain syndrome (CRPS), fibromyalgia, chronic widespread pain, chronic low back pain, and chronic pelvic pain.
Despite differences in origin or pathogenesis, chronic pain conditions are commonly associated with poor physical condition, fatigue, mobility limitations, depression, anxiety, sleep disturbances, and consequently reduced quality of life.
Sleep disturbances and fatigue are common symptoms in individuals with chronic conditions. Poor sleep worsens pain, stiffness, fatigue, and attention deficits.
How Is Chronic Pain Managed?
For many years, treatment for chronic pain focused on recommendations for rest and inactivity. However, exercise has been shown to offer significant benefits, including reducing pain severity and improving physical health and mood.
Chronic pain can be managed through pharmacological treatments as well as non-pharmacological approaches, such as physical activity (aerobic exercise, muscle strengthening, movement-based therapies).
Exercise programs prescribed by physiotherapists are increasingly promoted and implemented for a wide range of chronic pain conditions.
Physical activity improves:
-
Overall health (physical and mental)
-
Disease risk
-
Progression of chronic conditions (e.g. cardiovascular disease, type 2 diabetes, obesity)
Exercise prescribed by a physiotherapist significantly improves health outcomes and pain-related symptoms in chronic conditions, provided that appropriate parameters of frequency, duration, and intensity are applied. Regular movement is preferred over sedentary behavior. Exercise and muscle activation provide individuals with greater freedom and independence.
Note:
For exercise programs to be effective, they must be individually tailored by a physiotherapist, progress gradually, and take into account each person’s physical limitations as well as their psychosocial needs.
However, there is no better treatment for patients with chronic pain than empathy—the ability to place oneself in another’s position—and understanding from both the physiotherapist and the patient’s family.

